CRITICAL CARE TRIALS
Stay ahead of the curve with exciting new clinical trials from the critical care field presented in vivid, visual abstract format. Gain comprehensive and insightful perspectives as each critical development is delivered to you.
Mar 1, 2018
APROCCHSS Trial
Hydrocortisone plus Fludrocortisone for Adults with Septic Shock.
In a multicenter RCT of 1241 patients with septic shock, hydrocortisone plus fludrocortisone significantly reduced 90-day mortality compared to placebo (43.0% vs. 49.1%; P = 0.03) and improved ICU discharge, hospital discharge, and 180-day mortality rates. The intervention accelerated vasopressor weaning (17 vs. 15 vasopressor-free days; P < 0.001) and organ failure resolution (14 vs. 12 organ-failure-free days; P = 0.003). Hyperglycemia was more common, but serious adverse events were similar. These findings support hydrocortisone use for septic shock requiring vasopressors.
111
Feb 27, 2018
SMART Trial
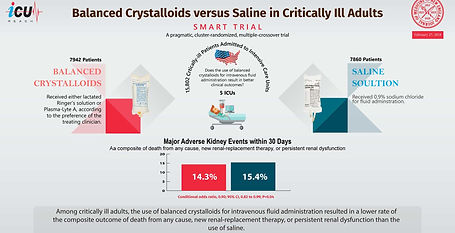
Balanced Crystalloids versus Saline in Critically Ill Adults
This pragmatic, cluster-randomized, multiple-crossover trial evaluated 15,802 critically ill adults admitted to five ICUs and compared the use of balanced crystalloids (lactated Ringer’s or Plasma-Lyte A) versus saline (0.9% sodium chloride) for intravenous fluid administration. The primary outcome was a composite of major adverse kidney events (MAKE) within 30 days, including death, new renal-replacement therapy, or persistent renal dysfunction. The incidence of MAKE was significantly lower in the balanced crystalloids group (14.3%) compared to the saline group (15.4%) with a marginal odds ratio of 0.91 (95% CI, 0.84–0.99; P=0.04). Secondary outcomes, including in-hospital mortality and new renal-replacement therapy, showed nonsignificant trends favoring balanced crystalloids. The study concluded that balanced crystalloids modestly reduced the risk of adverse kidney outcomes compared to saline in critically ill adults.
0
Feb 11, 2018
IDEAL-ICU
Timing of Renal-Replacement Therapy in Patients with Acute Kidney Injury and Sepsis.
In a multicenter RCT of 488 patients with septic shock and severe acute kidney injury, early initiation of renal replacement therapy (RRT) within 12 hours did not improve 90-day mortality compared to delayed initiation after 48 hours (58% vs. 54%; P = 0.38). Delayed RRT resulted in more RRT-free days (16 vs. 12 days; P = 0.006). Early RRT led to higher RRT use (97% vs. 62%; P < 0.001). These findings support delaying RRT unless emergent indications are present.
150
Dec 21, 2017
Culprit-SHOCK
PCI Strategies in Patients with Acute Myocardial Infarction and Cardiogenic Shock
In a multicenter RCT of 706 patients with acute MI and cardiogenic shock, culprit-lesion-only PCI significantly reduced the composite outcome of 30-day mortality or renal replacement therapy (45.9% vs. 55.4%; RR 0.83, 95% CI 0.71–0.96, P = 0.01) and 30-day mortality alone (43.3% vs. 51.6%; RR 0.84, 95% CI 0.72–0.98, P = 0.03) compared to multivessel PCI. Renal replacement rates and secondary outcomes were similar. Culprit-lesion-only PCI with staged revascularization is supported as the preferred approach.
81
Oct 10, 2017
ART Recruitment Trial
Effect of Lung Recruitment and Titrated Positive End-Expiratory Pressure (PEEP) vs Low PEEP on Mortality in Patients With Acute Respiratory Distress Syndrome
In a multicenter RCT of 1010 patients with moderate to severe ARDS, lung recruitment with PEEP titration by best respiratory-system compliance increased 28-day mortality compared to a low-PEEP strategy (55.3% vs. 49.3%; HR 1.20, 95% CI 1.01–1.42, P = 0.041). Secondary outcomes included higher 6-month mortality, fewer ventilator-free days, and increased risk of pneumothorax and barotrauma. Routine use of recruitment maneuvers is not supported, though subgroups may warrant further investigation.
253
Aug 3, 2017
ATHOS-3 Trial
Angiotensin II for the Treatment of Vasodilatory Shock.
In a multicenter RCT of 321 patients with catecholamine-resistant vasodilatory shock, angiotensin II significantly improved mean arterial pressure compared to placebo (69.9% vs. 23.4%; P < 0.001) and improved cardiovascular SOFA scores (−1.75 vs. −1.28; P = 0.01). Mortality at 28 days was not significantly different (46% vs. 54%; P = 0.12). While angiotensin II effectively raises blood pressure, further research is needed to assess its impact on patient-centered outcomes before widespread adoption.
158
Nov 1, 2016
HYPRESS Trial
Effect of Hydrocortisone on Development of Shock Among Patients With Severe Sepsis.
In a multicenter RCT of 380 patients with severe sepsis but not septic shock, early hydrocortisone use did not significantly reduce progression to septic shock within 14 days compared to placebo (21.2% vs. 22.9%; P = 0.70). Mortality, secondary infections, weaning failure, and muscle weakness were similar between groups, though hyperglycemia was more common with hydrocortisone (90.9% vs. 81.5%; P = 0.009). These findings do not support routine early hydrocortisone use in severe sepsis.
92
Aug 2, 2016
VANISH Trial
Effect of Early Vasopressin vs Norepinephrine on Kidney Failure in Patients With Septic Shock.
In a multicenter RCT of 409 septic shock patients, early vasopressin use (titrated up to 0.06 U/min) did not improve kidney failure–free days compared to norepinephrine (median 9 vs. 13 days; difference −4 days, 95% CI ��−11 to 5). Vasopressin was associated with reduced renal replacement therapy (25.4% vs. 35.3%; difference −9.9%, 95% CI −19.3% to −0.6%) but no difference in mortality or serious adverse events. These findings do not support vasopressin as first-line therapy over norepinephrine, though potential benefits warrant further study.
244
Jul 14, 2016
AKIKI Trial
Initiation Strategies for Renal-Replacement Therapy in the Intensive Care Unit.
In a multicenter RCT of 620 critically ill patients with severe acute kidney injury, early initiation of renal replacement therapy (RRT) did not improve 60-day mortality compared to delayed initiation (48.5% vs. 49.7%; P = 0.79). Nearly half of the delayed group avoided RRT entirely. Early RRT was associated with higher rates of catheter-related bloodstream infections (10% vs. 5%; P = 0.03). Findings support delaying RRT initiation unless clear indications are present.
107
Jun 4, 2015
FLORALI Trial
High-Flow Oxygen through Nasal Cannula in Acute Hypoxemic Respiratory Failure
In a multicenter RCT of 310 ICU patients with nonhypercapnic acute hypoxemic respiratory failure, high-flow oxygen therapy did not significantly reduce 28-day intubation rates compared to standard oxygen or noninvasive ventilation (38% vs. 47% and 50%; P = 0.18). However, high-flow oxygen improved ventilator-free days (24 vs. 22 vs. 19; P = 0.02) and lowered 90-day mortality (HR 2.01 vs. standard, P = 0.046; HR 2.50 vs. NIV, P = 0.006). Further large-scale studies are needed.
580
May 20, 2015
PermiT Trial
Permissive Underfeeding or Standard Enteral Feeding in Critically Ill Adults
In a multicenter RCT of 895 critically ill patients, permissive underfeeding (40–60% of calorie goals) did not reduce 90-day mortality compared to standard feeding (27.2% vs. 28.9%; RR 0.94, 95% CI 0.76–1.16; P = 0.58). Secondary outcomes, including ICU- and ventilator-free days, were similar. Post-hoc analysis suggested lower renal replacement therapy rates with permissive underfeeding (7.1% vs. 11.4%; P = 0.04). Permissive underfeeding is safe but does not offer clear survival benefits.
55
Apr 2, 2015
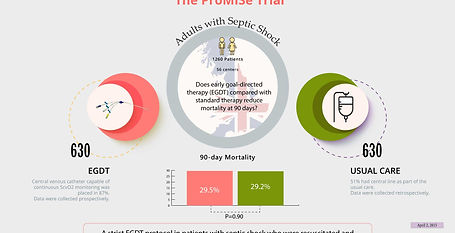
ProMISe Trial
Trial of Early, Goal-Directed Resuscitation for Septic Shock.
In a multicenter RCT of 1260 patients with septic shock, early goal-directed therapy (EGDT) did not reduce 90-day mortality compared to usual care (29.5% vs. 29.2%; P = 0.90). EGDT required greater treatment intensity, with more fluids, vasopressors, and transfusions, but showed no benefit in organ support, ICU/hospital stay, or quality of life. EGDT increased costs without cost-effectiveness. These findings support focusing on adequate fluid resuscitation and early antibiotics rather than strict EGDT protocols.
67