Advanced CT Perfusion Imaging in Stroke Management: A Detailed Insight
- Mazen Kherallah

- May 7, 2024
- 3 min read
Stroke, a leading cause of disability and mortality worldwide, is a complex medical condition where rapid and accurate diagnosis is crucial for effective management. CT perfusion is an invaluable tool in this setting, offering precise quantification of cerebral blood flow disruptions and helping differentiate between the ischemic penumbra and the infarct core. This post explores CT perfusion's critical role in acute stroke management, emphasizing the interpretation of cerebral blood flow (CBF), cerebral blood volume (CBV), mean transit time (MTT), and time to peak (TTP) values in differentiating reversible from irreversible cerebral ischemia.
CT Perfusion Technique: A Primer
CT perfusion involves the injection of iodinated contrast material and rapid serial imaging to assess the dynamics of cerebral blood flow. Accurate positioning and timing of the scan are crucial to ensure the reliability of the data. Key steps include:
Patient Positioning: Patients are placed supine with the head secured in a chin tuck position to minimize radiation to the eyes and ensure stability throughout the scanning process.
Contrast Administration: A rapid injection of contrast, typically at a rate of 6-8 mL/s, followed by a saline flush, is critical for optimal visualization of blood flow dynamics.
Scanning Protocol: The scan covers essential brain regions, typically focusing on the basal ganglia (anterior circulation), with a shuttle scan range of about 10 cm, adjusting as necessary based on the suspected location of ischemia.
Key Parameters Assessed in CT Perfusion
The primary parameters measured include:
Cerebral Blood Flow (CBF): Indicates the volume of blood flowing through a given mass of brain tissue per minute. Typically ranges from 50 to 60 milliliters per 100 grams of brain tissue per minute in the gray matter.
Cerebral Blood Volume (CBV): Represents the total amount of blood within the brain tissue. Generally around 4 to 5 milliliters per 100 grams of gray matter brain tissue.
Mean Transit Time (MTT): Reflects the average time it takes for blood to traverse the brain's vasculature. Usually falls between 4 to 6 seconds in the gray matter.
Time to Peak (TTP): The duration until the contrast agent reaches its peak concentration in the brain following its injection. Typically observed between 15 to 25 seconds, depending on the specific circulation dynamics and injection protocol.
Step-by-Step Interpretation Process
Initial Assessment:
Obtaining Values: The first step involves obtaining MTT, CBV, and CBF values from multiple regions of interest across both the affected and normal hemispheres. This comprehensive collection of data ensures a baseline is set for comparison.
MTT Evaluation: MTT is assessed next. A prolonged MTT compared to the normal hemisphere indicates that ischemia or infarction is present, suggesting a disruption in normal blood flow patterns.
Differentiating Tissue States:
Comparing CBF and CBV: To distinguish between ischemic and infarcted tissues, the values of CBF and CBV are critically compared:
Reversible Ischemia: If CBF is reduced but CBV is normal or slightly reduced, it suggests that the tissue ischemia might still be reversible. This indicates that while blood flow is compromised, enough blood volume remains to potentially salvage the tissue.
Irreversible Infarction: Markedly reduced CBF and CBV or non-measurable TTP point towards irreversible infarction. This suggests severe ischemia with substantial reduction in blood volume and flow, likely leading to tissue death.
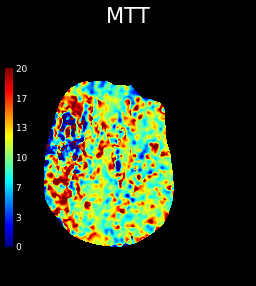
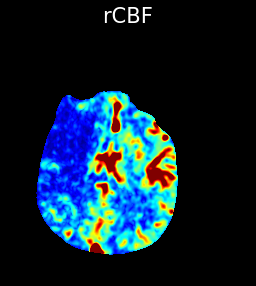
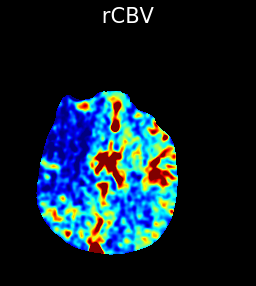
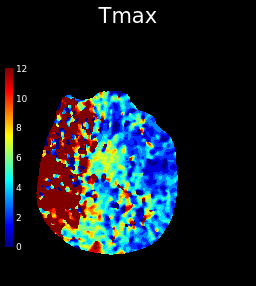
The above images depict a case of right MCA infarction, showing a prolonged MTT and markedly reduced CBF and CBV compared to the left side indicating a lack of significant blood flow reaching the tissue in the mCA distribution .
Practical Implications for Stroke Management
Clinical Decision-Making: These measurements are instrumental in guiding acute stroke management. Identifying areas of reversible ischemia enables timely interventions, such as thrombolytic therapy, which can restore blood flow and prevent permanent damage.
Prognostication: Knowing the extent of potentially salvageable brain tissue versus infarcted tissue helps in prognostication and planning appropriate post-stroke care and rehabilitation.
Conclusion
Through the nuanced interpretation of MTT, CBF, and CBV, CT perfusion imaging becomes a powerful tool in the differential diagnosis of ischemic stroke, allowing clinicians to make informed decisions about urgent interventions. This advanced capability not only helps in optimizing treatment strategies but also significantly impacts patient outcomes by facilitating targeted therapies based on specific perfusion patterns within the brain.








Comments